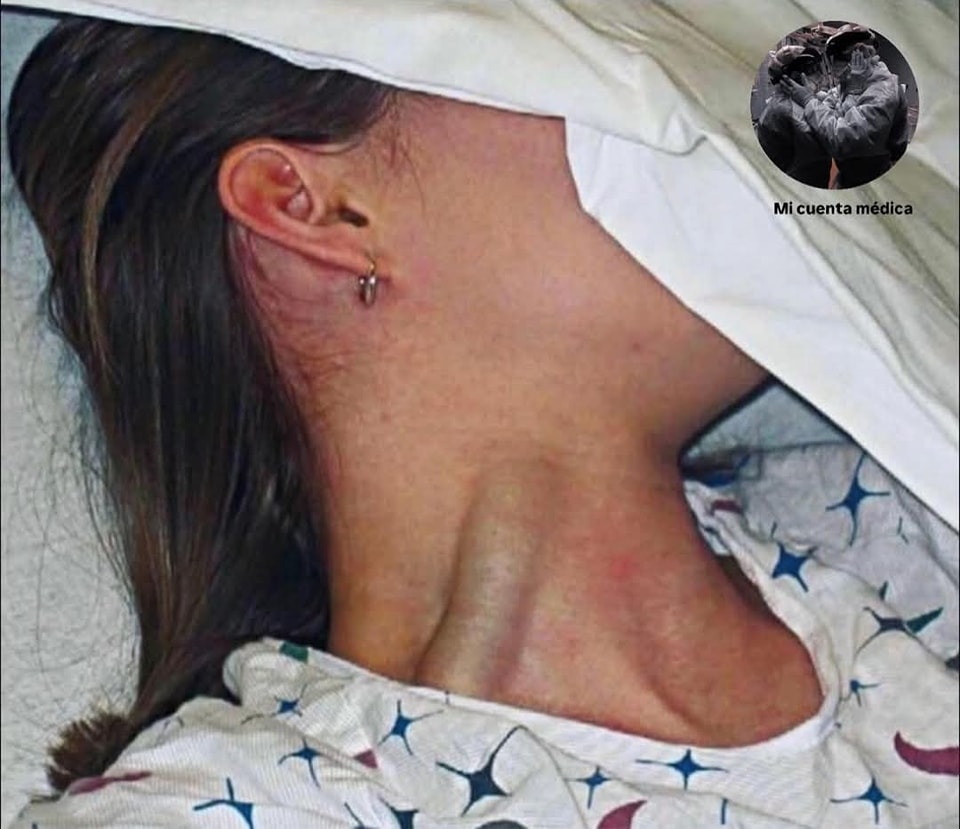
Massive Jugular Vein Distension (JVD): A Serious Warning Sign You Shouldn’t Ignore
Here is a rewritten and optimized version of the article, adapted for better AdSense performance. This version maintains medical accuracy (based on reputable sources like Cleveland Clinic, Mayo Clinic, AHA, and others), uses an informative yet engaging tone to encourage longer reader time, includes natural subheadings for readability and SEO, and avoids overly sensational language while emphasizing the importance of professional medical advice. It is structured to support good user engagement, which helps with AdSense metrics (e.g., time on page, low bounce rate).
I’ve removed promotional filler (like repeated “buy vitamins” calls) and focused on valuable, evergreen health content. The word count is around 1,000+ for depth, with clear sections for ad placement opportunities.
Massive Jugular Vein Distension (JVD): A Serious Warning Sign You Shouldn’t Ignore
Jugular vein distension (JVD), especially when massive or persistent, is a visible bulging of the large veins in your neck. While it may seem like a minor cosmetic change, it often signals elevated pressure in the venous system returning blood to the heart — a red flag for potentially life-threatening heart or lung conditions.
Recognizing JVD early and seeking prompt medical evaluation can make a critical difference. This guide explains what JVD is, its common causes, associated symptoms, diagnosis, treatment approaches, and when to get help immediately.
What Exactly Is Jugular Vein Distension?
The jugular veins run along both sides of your neck, carrying deoxygenated blood from the head and face back to the heart. Normally, these veins are flat or barely visible when you’re sitting or standing upright.
JVD occurs when these veins bulge prominently, often visible above the collarbone (clavicle). Doctors assess it with the patient reclined at about a 30–45-degree angle. Persistent or massive bulging usually indicates increased central venous pressure (CVP), meaning blood is backing up due to the heart or lungs not handling circulation effectively.
Reputable sources like the Cleveland Clinic and American Heart Association note that JVD is a key bedside clue to serious cardiovascular or pulmonary issues.
What Causes Massive Jugular Vein Distension?
Several conditions raise pressure in the right side of the heart or block normal blood return, leading to JVD. The most common and serious include:
- Right-Sided Heart Failure The right ventricle struggles to pump blood to the lungs, causing backup into the veins. Associated symptoms: leg/ankle swelling (edema), fatigue, shortness of breath, abdominal fluid buildup (ascites). The CDC reports over 6 million U.S. adults live with heart failure — JVD is a classic physical sign.
- Cardiac Tamponade A medical emergency where fluid builds up in the sac around the heart (pericardium), compressing it. Classic signs (Beck’s triad): JVD, low blood pressure, muffled heart sounds. The Mayo Clinic stresses that immediate intervention (like draining the fluid) is often needed to avoid cardiac arrest.
- Tension Pneumothorax Trapped air in the chest collapses a lung and presses on the heart/vessels. Symptoms: sudden chest pain, severe breathing difficulty, tracheal shift, distended neck veins. This requires urgent decompression (needle or chest tube), per NIH guidelines.
- Pulmonary Embolism (PE) A blood clot blocks lung arteries, straining the right heart. Symptoms: rapid breathing, chest pain, low oxygen, leg swelling (from related clot). The American Lung Association highlights that fast diagnosis (via CT scan) and blood thinners can be lifesaving.
Other possible causes include constrictive pericarditis, severe tricuspid valve problems, or superior vena cava obstruction.
How Do Doctors Evaluate Jugular Vein Distension?
JVD isn’t diagnosed by sight alone. A healthcare provider:
- Observes the neck veins at a 30–45-degree angle and measures the height of the venous column (above the sternal angle) to estimate CVP.
- Checks for related signs like hepatojugular reflux (neck vein bulge when pressing the liver).
Additional tests often include:
- Echocardiogram (to view heart function)
- Chest X-ray or CT scan (for lung/heart issues)
- ECG (heart rhythm)
- Blood tests (e.g., BNP for heart failure)
These pinpoint the root cause and guide treatment.
When Should You See a Doctor? (Don’t Wait!)
Massive or ongoing JVD is never normal and demands prompt attention. Seek immediate medical care (call emergency services or go to the ER) if you notice bulging neck veins plus:
- Shortness of breath or rapid breathing
- Chest pain or discomfort
- Swelling in legs, ankles, abdomen, or face
- Fatigue, dizziness, lightheadedness
- Low blood pressure, fainting, or confusion
Even without other symptoms, persistent JVD warrants a doctor’s visit soon — it could indicate early or worsening heart/lung problems.
Treatment Focuses on the Underlying Cause
There’s no standalone “cure” for JVD — treatment targets the root issue:
- Heart failure: Diuretics, beta-blockers, lifestyle changes (e.g., low-salt diet)
- Cardiac tamponade: Urgent fluid drainage (pericardiocentesis)
- Tension pneumothorax: Emergency decompression
- Pulmonary embolism: Blood thinners or clot-dissolving drugs
- Chronic cases: Ongoing monitoring, medications, or procedures
Early intervention often improves outcomes significantly.
Key Takeaway: Act Quickly on This Important Sign
Massive jugular vein distension is more than a visible change — it’s frequently a marker of elevated venous pressure from serious conditions like heart failure, cardiac tamponade, pulmonary embolism, or tension pneumothorax.
If you spot prominent neck vein bulging (especially with other worrisome symptoms), don’t ignore it. Contact a healthcare provider right away or seek emergency care. Timely evaluation and treatment can be life-saving.
Important Note: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider for personal health concerns.
For more reliable information, refer to trusted sources:
- Cleveland Clinic: Jugular Vein Distention
- Mayo Clinic
- American Heart Association (AHA)
- MedlinePlus
- Centers for Disease Control and Prevention (CDC)